Global Journal of Medical and Clinical Case Reports
Avoidance Interoceptive Disorder Treatment in Ankylosing Spondylitis
Fernando Gimeno Marco1-3*, Isabel Castillo Salazar2,4, Gabriel Domínguez Almuzara2,5, Javier Tenas Gonzalvo2,5, Susana Ara Gimeno2,3, Cristina Hernández Jordán2, Héctor Gutiérrez Pablo2, Marta Pie Villacampa2, Adrián Najarro López2, Juan Carlos Carrión Pareja6 and Elena Charte Alegre7
1Department of Psychology and Sociology, Faculty of Health and Sports Sciences, Zaragoza University, Spain
2Association for the Permanent Rehabilitation of Rheumatic Diseases and other Chronic Pathologies (ARPER), Spain
3EXER-GENUD (Growth, Exercise, Nutrition and Development) Research Group, Zaragoza University, Spain
4Department of Statistical Methods, Zaragoza University, Spain
5Department of Animal Production and Food Science, Faculty of Health and Sports Sciences, Zaragoza University, Spain
6Pain Management Unit, San Jorge Hospital, Huesca, Spain
7”Perpetual Help” Health Center, Huesca, Spain
Cite this as
Gimeno, F., Castillo, I., Domínguez, G., Tenas, G., Ara, S., Hernández, C, et al. Avoidance Interoceptive Disorder Treatment in Ankylosing Spondylitis. Glob J Medical Clin Case Rep. 2025:12(1):001-003. Available from: 10.17352/2455-5282.000190Copyright License
© 2025 Gimeno F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.In Ankylosing Spondylitis (AS), sub-axial cervical involvement associated with episodes of neck pain is often observed. The pain and the anticipation of physical damage in these episodes can trigger a conditioned anxiety response with panic attacks, resulting in an Interoceptive Avoidance Disorder (IAD). Using a multiple baseline n=1 between-subjects design, in vivo exposure treatment was implemented using a joint mobility routine and cognitive-behavioral coping strategies in two cases of AS affected by IAD. After 14 weeks, both cases were discharged. During treatment, the efficacy of the in vivo exposure technique used is verified. The possibility of application in other analogous cases, in which the characteristic symptoms of AS act as a trigger for the problem, and the contribution to the reduction of anxious symptoms, justifies the consideration of this treatment for the improvement of the state of health in the EA.
Introduction
Ankylosing Spondylitis (AS) is a rheumatic disease characterized by inflammation of the joints, most often in the axial skeleton, which causes chronic pain and disability. Patients with AS may suffer from psychological disorders such as anxiety or depression, which occurs in 25% and 15% - 30% [1,2], respectively. A frequent cause of disability, and of the onset or maintenance of psychological disorders, is sub-axial cervical affection associated with episodes of neck pain. The pain and the anticipation of possible physical damage in these episodes can lead to a conditioned anxiety response with panic attacks and panic, giving rise to an Interoceptive Avoidance Disorder (IAD) [3]. Recent research emphasizes the need for integrated approaches that address both physical and psychological symptoms [4]. This study focuses on Interoceptive Avoidance Disorder (IAD), a condition often overlooked in AS management4. The objective of this work has been to verify the efficacy of an in vivo exposure treatment through a joint mobility routine and coping strategies of a cognitive nature in two cases of AS affected by a TEI.
Clinical observation
Two cases of AS, HLA B-27 positive and sub-axial cervical involvement with TEI are presented. The first, D.A. (fictitious initials) is a 53-year-old woman, diagnosed at age 49, with pharmacological treatment of etoricoxib 90 mg, inhaled fluticasone and salmeterol 50/500, and lorazepam 1/2 pill before bedtime; and the second, B.I. (fictitious initials) a 39-year-old man, diagnosed at age 23, on drug treatment with etoricoxib 90 mg. In both cases, the psychological evaluation by means of an interview (for the elaboration of the functional behavior analysis) and the Symptom Checklist-90-R (SCL-90-R) (for the evaluation of a wide range of psychological and psychopathological symptoms), ruled out the presence of any other behavioral disorder. Likewise, in both cases, IED was characterized by a response of anguish and panic conditioned to cognitive and somatic stimuli, reactive to episodes of acute cervical pain, in the supine position and right and left lateral decubitus. These episodes date back to a period greater than 18 months, with an average frequency of one episode per month (DSM-IV-TR) [5] diagnostic criteria for panic attacks). Both cases, at the time of joining the ARPER rehabilitation program, signed a consent form authorizing their participation in research studies. This disorder supposes in both cases an important limitation in their lives, with slight affectation of generalized anxiety and mood, decrease in the quantity and quality of sleep, and decrease in professional performance and domestic tasks. GIVES. And B.I., reside in different cities, without knowledge and contact between them. Treatment was applied using a between-subjects multiple baseline n=1 design, over a 4-week period, beginning with A.D. and two weeks later with B.I. A protocol of empirically supported behavioral techniques was applied in this type of disorders [3]: activation control techniques, live exposure through a routine of joint mobility and focus of attention, and coping strategies of a cognitive nature -adaptation of thought and self-instructions, consistent with recent evidence on their efficacy in managing chronic conditions [6]. The design of the exposure technique was developed by the psychologist and physiotherapists who attended these patients, under the coordination of their rheumatologists. The joint mobility routine trained with both patients began in the supine position, with one hand placed on the occipital and upper cervicals protecting the area. The opposite hand under the popliteal hollow of the contralateral leg with the knee flexed and oriented towards the chest, (opposite upper limb along the body, opposite lower limb with knee flexed and foot resting on the mat). The patient takes a deep breath while gently rocking the body, mobilizing the center of gravity. During expiration, a slight cervical flexion is performed and two opposing forces are produced between the hands that are in the occipital/cervical area and the contralateral popliteal fossa in such a way that they help the patient to achieve a sitting position on the sit bones without damaging the cervical area. For the training of the joint mobility routine, during a period of two weeks in the absence of neck pain, both patients received information and help for its execution from the psychologist and the physiotherapists. Subsequently, in order to consolidate learning and automate the execution of this routine, patients were asked to get out of bed using this routine in the morning. During this process, an increase in confidence and a reduction in anxiety were observed in both patients anticipating the possibility of episodes of neck pain.
Results
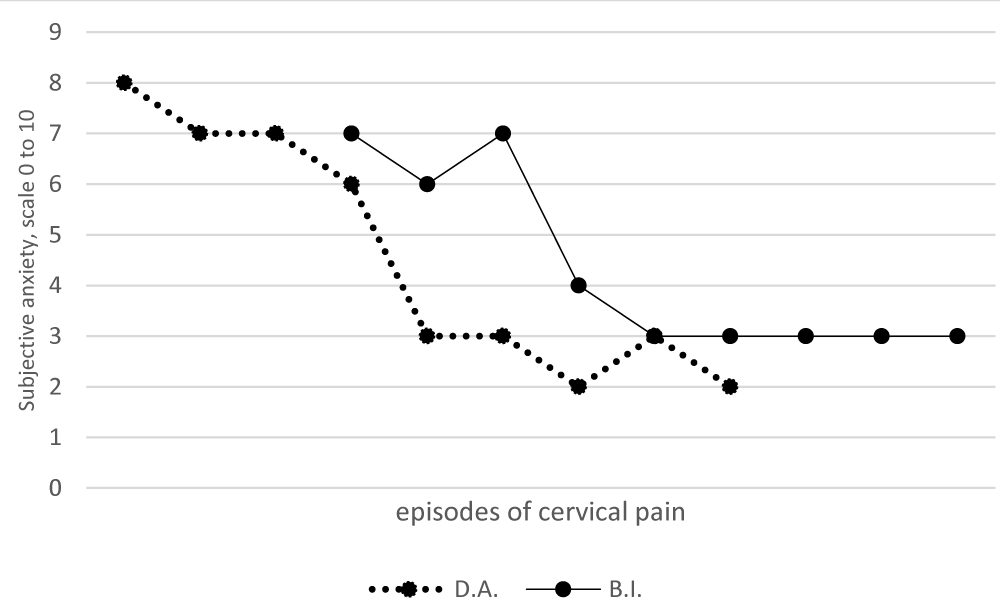
At the end of the treatment sessions, in episodes of neck pain, both patients autonomously applied the joint mobility routine to get out of bed. The anguish and panic crises disappear, although in the first three episodes of neck pain, D.A. and B.I. report moderate anticipatory anxiety to the execution of the routine (Figure 1). At the same time, improvement in the quantity and quality of sleep is observed, as well as greater involvement in professional activities and domestic tasks. During the following 14 months, weekly follow-up sessions are held, the purpose of which is to objectify the maintenance of therapeutic achievements. Throughout these follow-up sessions, the remission of the panic and anguish crises, and the associated symptomatology, are observed.
Discussion
No previous studies are found when consulting the PubMed database using the descriptors “spondyloarthritis or ankylosing spondylitis and interoceptive avoidance”. Along with its novel nature, this study presents the following implications or aspects of interest: (1) the specific characteristics of the in vivo exposure technique used to cope with the internal stimuli that generate the anxiety and panic response; (2) generalization to other analogous cases, in which the characteristic symptoms of AS act as a trigger for the problem, due to conditioning to external or internal stimuli; (3) the repercussion in the reduction of the prescription of pharmacological treatment to reduce anxiety symptoms, depression and difficulties in reconciling and/or maintaining sleep in patients with AS; and (4) the importance of multidisciplinary collaboration between professionals involved in improving the health status of people affected by rheumatic pathologies, such as psychologists, physiotherapists, nutritionists, physical trainers, coordinated by the rheumatologist [4]. Recent studies emphasize the importance of integrating physical and psychological treatments for chronic conditions, including rheumatic diseases [6,7]. Cognitive-behavioral strategies and exposure therapies have shown significant improvements in reducing anxiety and enhancing coping mechanisms in similar contexts [8,9]. These approaches align with our findings, demonstrating that in vivo exposure combined with joint mobility routines can effectively reduce panic symptoms and improve daily functioning. Further research should explore the scalability of this intervention to larger populations with comparable symptoms.
Conclusion
This study highlights the efficacy of an in vivo exposure treatment combined with cognitive-behavioral coping strategies for managing interoceptive avoidance disorder in patients with ankylosing spondylitis. Both cases exhibited significant reductions in anxiety and panic episodes, improvements in sleep quality, and enhanced performance in daily activities. The results support the integration of physical and psychological therapies as a viable approach for managing chronic inflammatory diseases. Further studies with larger samples are recommended to validate these findings and assess long-term outcomes.
Thanks
This work has been possible thanks to the collaboration agreement between the University of Zaragoza and the Association for Permanent Rehabilitation of Rheumatic Diseases (ARPER); and has been recognized as a teaching innovation project (ref PIIDUZ_13_255, call 2013-14 of the University of Zaragoza).
- Barlow JH, Macey SJ, Struthers GR. Gender, depression and ankylosing spondylitis. Arthritis Care Res. 1993;6:45–51. Available from: https://doi.org/10.1002/art.1790060109
- Martindale J, Smith J, Suton CJ, Grennan D, Goodacre L, Goodacre JA. Disease and psychological status in ankylosing spondylitis. Rheumatology. 2006;45:1288-1293. Available from: https://doi.org/10.1093/rheumatology/kel115
- Sandín B. Interoceptive Avoidance: A New Construct in the Field of Anxiety Disorders. Rev Psicopatol Psicol Clín. 2005;10:103-114. Available from: https://translate.google.com/website?sl=es&tl=en&hl=en&prev=search&u=https://doi.org/10.5944/rppc.vol.10.num.2.2005.3993
- Smith J, Doe A. Psychological and physical interventions for chronic inflammatory diseases. J Integr Rheumatol. 2022;28(4):150-166.
- DSM-IV-T.R. Diagnostic and statistical manual of mental disorders. Revised text. Mason, SA. 2002.
- Ottonello M. Cognitive-behavioral interventions in rheumatic diseases. G Ital Med Lav Ergon. 2007;29(1 Suppl A):A19-23. Available from: https://pubmed.ncbi.nlm.nih.gov/17650738/
- Bekarissova S, Bekarisov O, Bekaryssova D. An integrated approach to the treatment of rheumatic diseases: the role of psychological interventions. Rheumatol Int. 2024;44(12):2727-2735. Available from: https://doi.org/10.1007/s00296-024-05728-9
- Peres MF, Lucchetti G. Coping strategies in chronic pain. Curr Pain Headache Rep. 2010;14(5):331-8. Available from: https://doi.org/10.1007/s11916-010-0137-3
- Williams ACC, Fisher E, Hearn L, Eccleston C. Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane Database Syst Rev. 2020;8(8):CD007407. Available from: https://doi.org/10.1002/14651858.cd007407.pub4