Global Journal of Medical and Clinical Case Reports
Association between Complicated Pneumonia and Viral Pericarditis in a Pediatric Patient: Case Report
Ricardo Sánchez Algarín1*, Angélica María Mendoza Caballero1, Patricia Romero Luzardo1, Lupo Ramón Méndez Durán2 and Richard Germán Romero Ruiz3
1Department of Pediatrics, Colombia
2Department of Pediatric Cardiology, Colombia
3Department of Pediatric Intensive Care, Colombia
ORCiD : Angélica María Mendoza Caballero - https://orcid.org/0009-0007-9138-2997
ORCiD : Patricia Romero Luzardo - https://orcid.org/0009-0008-2718-3157
ORCiD : Richard Germán Romero Ruiz - https://orcid.org/0009-0005-0352-6651
Cite this as
Algarín RS, Mendoza Caballero AM, Luzardo PR, Méndez Durán LR, Romero Ruiz RG. Association between Complicated Pneumonia and Viral Pericarditis in a Pediatric Patient: Case Report. Glob J Medical Clin Case Rep. 2025:12(1):018-021. Available from: 10.17352/2455-5282.000193Copyright License
© 2025 Algarín RS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The coexistence of complicated pneumonia and viral pericarditis in a pediatric patient is a rare clinical scenario that presents diagnostic and therapeutic challenges. This case involves a 14-year-old adolescent who was admitted with symptoms of general discomfort, fever, cough, and difficulty breathing. Initial evaluation revealed pulmonary parenchymal consolidation, an enlarged cardiac silhouette, and pleural effusion on radiographic imaging, leading to the initial diagnosis of complicated pneumonia. However, due to the clinical presentation and the finding of cardiomegaly, an echocardiogram was performed, confirming the diagnosis of pericarditis. Specific viruses (rhinovirus and enterovirus) were identified as the etiological agents. The combination of complicated pneumonia and viral pericarditis represents a significant clinical challenge that requires a comprehensive evaluation and a collaborative multidisciplinary approach.
Introduction
Pneumonia complications occur when the infection extends beyond the pulmonary parenchyma to neighboring areas or when the infection develops more complexly due to various factors [1]. However, these complications are observed in only 1% of cases, rising to 40% in patients requiring inpatient management. Treatment is nonspecific and directed at the particular complication, which may include Parapneumonic Pleural Effusion (PPE), Pulmonary Empyema (PE), pneumothorax, Bronchopleural Fistula (BPF), pulmonary abscess (PA), Necrotizing Pneumonia (NP), or pyopneumothorax [2].
Viral pathogens are significantly frequent and potentially underestimated etiological agents in such clinical presentations in pediatric patients. In fact, complicated hospital-acquired types of pneumonia not related to mechanical ventilation are associated with viral pathogens in 22% of cases. Among these, the most commonly identified agents include rhinovirus, influenza, and parainfluenza viruses [3]. Enteroviruses, though less common, may also contribute to such cases due to multisystemic viral dissemination following viremia.
Pericarditis, on the other hand, is one of the most common cardiac conditions characterized by inflammation of the pericardial layers. Its reported incidence in the general population is 30-150 cases per 100,000 per year and accounts for <0.2% to 5% of all emergency department visits for chest pain in children without prior cardiac disease [4]. In developed countries, viral infections are the most commonly identified etiology, whereas Tuberculosis (TB) predominates in developing regions [5]. According to a study by Shakti D., the most frequent causes of pericarditis and pericardial effusions in hospitalized pediatric patients include post-cardiac surgery (54%), neoplasms (13%), and renal disease (13%), while idiopathic or viral pericarditis (5%) and rheumatologic causes (5%) are less common underlying etiologies. Most current treatment strategies for pediatric pericarditis are derived from adult data [6].
This case report documents an exceptional clinical scenario involving the development of complicated pneumonia with the coexistence of pleural effusion, pericardial effusion, and pericarditis. This posed significant diagnostic and therapeutic challenges, requiring a comprehensive evaluation and multidisciplinary approach, ultimately leading to a favorable resolution of the associated pathologies.
The objective of this case report is to provide a detailed description of this unusual clinical presentation, its diagnosis, treatment, and patient outcomes while highlighting the importance of a multidisciplinary approach. Furthermore, the report underscores the need for increased investigative focus to better understand the clinical implications of this uncommon combination of conditions.
Case report
A 14-year-old female adolescent with a history of autism spectrum disorder grade 1 (“needs notable help”) without mention of immunosuppression states or alterations in their immune system previously, managed solely with risperidone to treat episodes of insomnia in addition to cognitive behavioral therapy, presented with a clinical course that began two weeks before her emergency department visit. Her symptoms included episodes of dry cough accompanied by tachypnea, tachycardia, general malaise, and unquantified fever spikes. She experienced respiratory deterioration associated with the reduced functional class due to moderate-effort dyspnea and persistent febrile episodes.
Upon admission, her vital signs were as follows: blood pressure of 105/60 mmHg, heart rate of 155 bpm, respiratory rate of 45 breaths per minute, oxygen saturation of 95% on room air, and a temperature of 37.6 °C. Regarding her anthropometric measurements, she was 152 cm tall and weighed 43 kg with a body mass index of 18.6, which classifies her as a teenager in height and mass index appropriate for her age. Physical examination revealed respiratory distress with subcostal and intercostal retractions. Auscultation showed diminished vesicular breath sounds with bibasilar crackles, low-intensity rhythmic heart sounds with a fourth heart sound, apex beat, and an antalgic squatting position.
Laboratory workup included a complete blood count, revealing moderate anemia (hemoglobin: 8.1 g/dL, hematocrit: 25.8%), leukocytosis with a left shift (white blood cells: 21,400 cells/μL, neutrophils: 64.9%), thrombocytosis (platelets: 1,076,000/μL), and elevated C-reactive protein (30.9 mg/L). Electrolytes, renal function, and coagulation times were within normal limits.
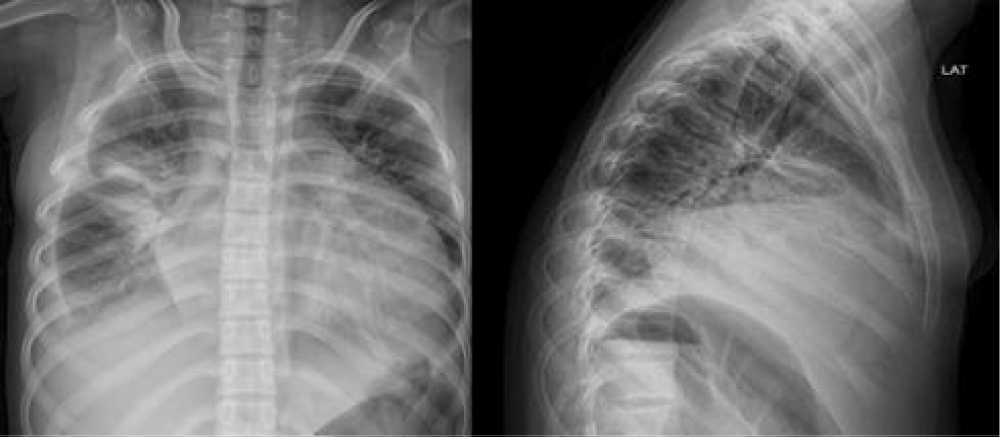
Chest X-rays (Images 1,2) showed homogeneous radiopacity in the middle lobe, obliteration of the right costophrenic angle, and cardiomegaly. A pleural ultrasound revealed bilateral pleural effusion, predominantly on the right side, with an estimated volume of 750 mL on the right and 67 mL on the left.
She was admitted to the Pediatric Intensive Care Unit (PICU), requiring oxygen therapy and a dual broad-spectrum antibiotic regimen consisting of a third-generation cephalosporin (ceftriaxone at 100 mg/kg/day) and a lincosamide (clindamycin at 40 mg/kg/day), given the diagnosis of complicated pneumonia with pleural effusion.
A subsequent chest computed tomography (Image 3) revealed parenchymal involvement consistent with consolidation in the right middle and lower lobes, along with pleural and pericardial effusions. A transthoracic Doppler echocardiogram was performed, which showed a grade III pericardial effusion (5 cm separation of pericardial layers) with significant hemodynamic compromise, partial collapse of the right-sided cardiac chambers, and moderate contractile dysfunction.
The patient underwent intervention with a pericardial window and closed thoracostomy for drainage obtaining a turbid fluid during the procedure.
In suspected pyogenic pericarditis due to Pseudomonas, empirical antibiotic coverage was initiated with piperacillin-tazobactam at 400 mg/kg/day. After 72 hours of stay, blood cultures, pleural fluid, and pericardial fluid cultures were negative, PCR for Mycobacterium was not detected, PCR for COVID-19 was negative, and FilmArray was positive for Rhinovirus and Enterovirus, so the clinical picture was considered to have a viral etiology.
After consulting with the Infectious Disease service, it was decided to continue antibiotic treatment for 15 days, with a follow-up echocardiogram showing no residual pericardial effusion, normal-sized cardiac chambers, and preserved contractile function.
Due to an adequate clinical, biochemical, and imaging response to the established medical management, discharge was recommended with ongoing interdisciplinary outpatient follow-up by the pediatric, cardiology, and pediatric infectious disease services.
Discussion
The concomitance of complicated pneumonia and viral pericarditis in a patient represents a unique clinical situation that combines respiratory and cardiac conditions [1]. Both are inflammatory processes with multiple etiologies and although the medical literature mentions various causes for acute pericarditis, especially viral infections like influenza and coxsackie, the association between pericarditis and complicated pneumonia is very rare, occurring in less than 5% of reported cases. Of these, most mention the association of complicated pneumonia and bacterial pericarditis with the characteristic presentation of purulent pericarditis, as seen in the report published by Tenenbaum T [7], which mentions this relationship between the described pathologies with a bacterial origin caused by Chlamydophila pneumoniae.
It is important to highlight that following the conditions observed during the pandemic, studies evaluating pericardial disease among children with COVID-19 are limited to small case reports [8]. Among these, acute pericarditis and pericardial effusion with tamponade have been described in children with COVID-19, noting that typical respiratory symptoms were not present [9].
The overlap of symptoms and clinical findings between both conditions can complicate the accurate diagnosis. Patients may present chest pain, fever, shortness of breath, and other symptoms that could be attributed to both pneumonia and pericarditis [10]. Therefore, it is crucial to perform comprehensive diagnostic tests, including blood analysis, imaging studies, and cardiac and pulmonary function tests, to properly differentiate and characterize both conditions [11].
A thorough literature review was conducted, and no cases were found that mentioned viral pericarditis as a complication of pneumonia. However, it is important to emphasize that when isolated pericarditis is discussed, the most frequent etiology is viral in origin. This is due to the fact that most pericarditis cases are idiopathic [12], and they are often attributed to a viral component, frequently without isolating the associated pathogen, because the vast majority of these conditions in pediatrics are self-limited, with a natural evolution similar to a viral infection without complications. However, when pericarditis is a consequence of complicated pneumonia, it is almost always described as having a bacterial origin, presenting as a purulent pericardial infection [13]. This is why it is striking that in our patient, the reports from cultures (blood cultures x2, cerebrospinal and pericardial fluid cultures, and cytology) were negative, so the instituted treatment was ineffective. Given the massive volume found in the echocardiogram with hemodynamic impact, our patient required intervention for fluid evacuation through a pericardial window and closed thoracostomy. A FilmArray was performed, reporting positive results for viral pathogens (Enterovirus – Rhinovirus). This shows that although most pericarditis cases, as mentioned earlier, resolve spontaneously and are idiopathic, this case required intervention to determine etiology after treatment with an adequate clinical response. Additionally, it is noteworthy that the echocardiogram described a grade III pericardial effusion that did not progress to cardiac tamponade, as would be expected due to the increased pressure on the heart muscle. This demonstrates the importance of prompt intervention to avoid complications such as heart failure, respiratory failure, and arrhythmias [14].
Regarding prognosis, the response to treatment and the recovery of patients depends on the severity of the disease, the speed at which the diagnosis is made, and the effectiveness of the treatment [15].
Conclusion
The combination of complicated pneumonia and viral pericarditis represents a significant clinical challenge that requires thorough evaluation and a collaborative approach across different medical disciplines. Accurately identifying the causes and administering timely treatment is essential to promote patient recovery and prevent potential long-term complications. This clinical case highlights the importance of recognizing and treating this unusual coexistence of pathologies to ensure the best possible care.
- Moreno-Pérez D, Andrés Martín A, Tagarro García A, Escribano Montaner A, Figuerola Mulet J, García García JJ, et al. Community acquired pneumonia in children: Outpatient treatment and prevention. An Pediatr (Barc). 2015;83(6):439.e1-7. Spanish. Available from: https://doi.org/10.1016/j.anpedi.2014.10.028
- Shorr AF, Zilberberg MD, Micek ST, Kollef MH. Viruses are prevalent in nonventilated hospital-acquired pneumonia. Respir Med. 2017;122:76-80. Available from: https://doi.org/10.1016/j.rmed.2016.11.023
- Yusuf SW, Hassan SA, Mouhayar E, et al. Pericardial disease: a clinical review. Expert Rev Cardiovasc Ther. 2016;14(4):525-39. Available from: https://doi.org/10.1586/14779072.2016.1134317
- Sogaard KK, Farkas DK, Ehrenstein V, Bhaskaran K, Botker HE, Sorensen HT. Pericarditis as a marker of occult cancer and a prognostic factor for cancer mortality. Circulation. 2017;136(11):996-1006. Available from: https://doi.org/10.1161/circulationaha.116.024041
- Shahid R, Jin J, Hope K, Tunuguntla H, Amdani S. Pediatric pericarditis: Update. Curr Cardiol Rep. 2023;25(3):157-70. Available from: https://doi.org/10.1007/s11886-023-01839-0
- Shakti D, Hehn R, Gauvreau K, Sundel RP, Newburger JW. Idiopathic pericarditis and pericardial effusion in children: contemporary epidemiology and treatment. J Am Heart Assoc. 2014;3(6):e001483. Available from: https://doi.org/10.1161/jaha.114.001483
- de Benedictis FM, Kerem E, Chang AB, Colin AA, Zar HJ, Bush A. Complicated pneumonia in children. Lancet. 2020;396(10253):786-98. Available from: https://doi.org/10.1016/s0140-6736(20)31550-6
- Raymond TT, Das A, Manzuri S, Ehrett S, Guleserian K, Brenes J. Pediatric COVID-19 and pericarditis presenting with acute pericardial tamponade. World J Pediatr Congenit Heart Surg. 2020;11(6):802-804. Available from: https://doi.org/10.1177/2150135120949455
- Dimopoulou D, Spyridis N, Dasoula F, Krepis P, Eleftheriou E, Liaska M, et al. Pericarditis as the main clinical manifestation of COVID-19 in adolescents. Pediatr Infect Dis J. 2021;40(5):e197-e199. Available from: https://doi.org/10.1097/inf.0000000000003096
- Krasic S, Prijic S, Ninic S, Borovic R, Petrovic G, Stajevic M, et al. Predictive factors of recurrence after pediatric acute pericarditis. J Pediatr (Rio J). 2021;97(3):335-341. Available from: https://doi.org/10.1016/j.jped.2020.06.007
- Lazarou E, Tsioufis P, Vlachopoulos C, Tsioufis C, Lazaros G. Acute pericarditis: Update. Curr Cardiol Rep. 2022;24(8):905-913. Available from: https://doi.org/10.1007/s11886-022-01710-8
- McGuire M, Harvey W, Brady T, Nguyen AD. Diagnosing and treating pericarditis and myocarditis in the emergency department. Emerge Med Prat. 2023;25(7):1-24. Epub 2023 Jul 1. Available from: https://pubmed.ncbi.nlm.nih.gov/37352407/
- Chiabrando JG, Bonaventura A, Vecchié A, Wohlford GF, Mauro AG, Jordan JH, et al. Management of acute and recurrent pericarditis: JACC state-of-the-art review. J Am Coll Cardiol. 2020;75(1):76-92. Available from: https://doi.org/10.1016/j.jacc.2019.11.021
- Welch TD, Oh JK. Constrictive pericarditis. Cardiol Clin. 2017;35(4):539-549. Available from: https://doi.org/10.1016/j.ccl.2017.07.007
- Imazio M, Brucato A, Pluymaekers N, Breda L, Calabri G, Cantarini L, et al. Recurrent pericarditis in children and adolescents: A multicenter cohort study. J Cardiovasc Med (Hagerstown). 2016;17(9):707-712. Available from: https://doi.org/10.2459/jcm.0000000000000300